Eyelids do far more than frame the eyes. They spread tears, shield delicate tissues, filter light, and help keep the surface of the eye comfortable. When something disrupts this system, whether it’s swelling, drooping, irritation, or a lump, the symptoms can feel surprisingly disruptive to daily life. Because eyelid issues can overlap with vision and tear problems, the best outcomes often come from understanding what is happening, what can be treated conservatively, and when a more targeted medical approach is appropriate.
How Doctors Narrow Down the Cause
A thorough evaluation usually starts with a detailed history of when symptoms began, what makes them worse, and whether there is pain, discharge, itching, or changes in vision. The examination often includes assessing eyelid position, blink completeness, tear film stability, and the lid margins where the glands open. Many clinics also use photographs and measurements to track changes over time. For complex eyelid alignment or reconstructive concerns that don’t respond to standard treatments, consulting an oculo plastic surgeon in Vadodara can provide specialized guidance and treatment options.
When Appearance and Function Intersect
Some eyelid disorders affect confidence, but their most important effects are functional: incomplete blinking can dry the eye, a turned-in eyelid can scratch the cornea, and heavy lids can narrow the visual field. Treatment planning often balances comfort, safety, and long-term stability. Options range from warm compresses and drops to procedures that adjust the lid margin or remove a lesion. A skilled clinician will explain what is medically necessary, what is elective, and what could change if left untreated.
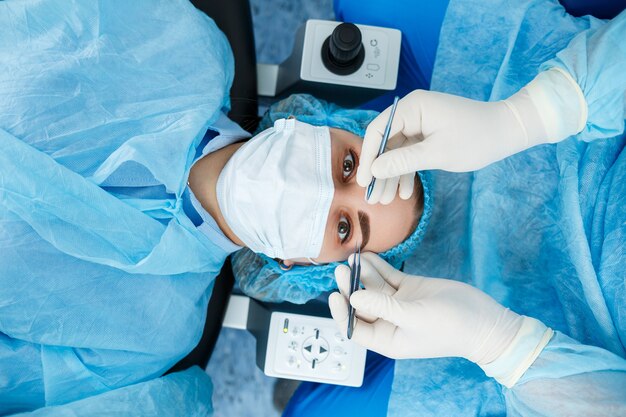
Common Lid Problems and What They Feel Like
Many conditions share similar symptoms: redness, swelling, foreign-body sensation, tearing, or intermittent blur. Styes and chalazia present as tender or firm bumps; blepharitis causes crusting and morning irritation; allergic eyelid inflammation often comes with itching; and lid malpositions can produce watering or scratchiness. Because signs overlap, self-diagnosis can lead to delayed care or overuse of topical products that irritate the skin. A structured approach makes it easier to match symptoms with an effective plan rather than guessing.
Everyday Measures That Often Help
Before medications or procedures, clinicians frequently recommend simple habits: consistent lid hygiene, gentle cleansing, warm compresses, and avoiding eye rubbing. Hydration, sleep, and limiting smoky or dusty exposure can reduce flare-ups in sensitive eyes. Contact lens users may need temporary breaks or changes in cleaning solutions. These steps are not “minor” when done consistently; for many people, they reduce recurrence and make other therapies work better. It’s also wise to review cosmetics and creams used near the lash line, since residues can block oil glands and worsen irritation.
Medicines and Office-Based Care
If home measures aren’t enough, treatment may include lubricating drops, anti-inflammatory agents, or short courses of antibiotic ointment when infection is suspected. Allergy-driven issues might respond to antihistamine drops or targeted anti-inflammatory therapy. In persistent bumps, clinicians may suggest injection therapy or a small drainage procedure in a controlled setting. This is where specialized eye treatments can be especially valuable, tailored to the lid’s anatomy and the eye surface, so that relief is achieved without creating new dryness or irritation.
Procedures That Restore Lid Position
When eyelids sit too low, roll inward, or sag outward, the eye surface can suffer. Ptosis repair may be considered when drooping blocks vision or causes brow strain. Entropion correction prevents lashes from rubbing the cornea, while ectropion repair helps the lid contact the eye properly and improves tear distribution. These procedures are usually customized to the cause of age-related tissue laxity, scarring, nerve issues, or prior surgery. Recovery plans often include cold compresses, prescribed ointment, and activity restrictions to support safe healing and predictable results.
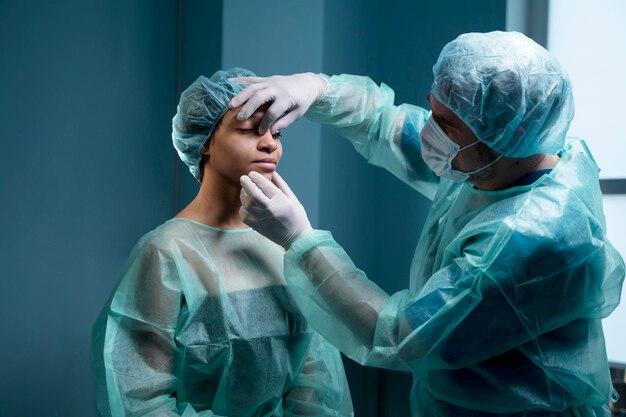
Managing Tear Drainage and Excess Watering
Watery eyes can be confusing because the cause may be dryness, irritation, or blocked drainage. Dry eyes can trigger reflex tearing, while narrowed tear ducts can cause overflow. Evaluation typically includes checking the puncta (drain openings), assessing lid position, and occasionally irrigating the tear ducts. By addressing the underlying issue, whether it’s enhancing tear quality, reducing inflammation, managing allergies, or correcting obstructions, patients can quickly improve eye health and regain daily comfort.
Lumps, Growths, and When to Be Cautious
Most eyelid lumps are benign, but any growth that changes quickly, bleeds, crusts persistently, or causes lash loss deserves prompt assessment. Doctors look at borders, color, ulceration, and how the lesion behaves over time. If something appears suspicious, a biopsy may be recommended. For benign lesions, removal can still be considered if they irritate the eye, interfere with blinking, or create recurrent inflammation. The key is ensuring the diagnosis is clear before treating, so that a harmless-appearing lesion does not mask a more serious condition.
Closing Thoughts
Eyelid and eye disorders often respond well when care is timely and targeted. The best plan typically combines careful diagnosis, consistent daily habits, and the right intervention, whether that is medication, an in-office procedure, or surgical correction. If symptoms persist, worsen, or begin to affect vision, seeking professional evaluation can prevent complications and improve eye health over the long term.



